The CV Event Risk graph displays your data as the % risk of a Cardiovascular Event in 5 years time. It is a guide only based on population health statistics and is useful for clinicians to gain a high level view of patients who are at risk for surveillance. It is derived from the publication "National Vascular Disease Prevention Alliance. Guidelines for the management of absolute cardiovascular disease risk. 2012" which is available from the websites of the members of the National Vascular Disease Prevention Alliance (Heart Foundation, National Stroke Foundation, Diabetes Australia and Kidney Health Australia).
About the Guidelines
The National Vascular Disease Prevention Alliance (NVDPA) The National Vascular Disease Prevention Alliance (NVDPA) includes the Heart Foundation, National Stroke Foundation, Kidney Health Australia and Diabetes Australia. Guidelines for the management of absolute cardiovascular disease risk has been developed through an evidence and consensus-based approach, and has received endorsement from the National Health and Medical Research Council.
The National Health and Medical Research Council–approved guidelines build on the cardiovascular disease (CVD) risk assessment guidelines, which introduced a new way of calculating CVD risk for people in Australia, released in 2009.
"Absolute cardiovascular risk assessment, using the Framingham Risk Equation to predict risk of a cardiovascular event over the next 5 years, should be performed for all adults aged over 45years without existing CVD or not already known to be at increased risk of CVD. Commence assessment in Aboriginal and Torres Strait Islander adults at 35 years."
In the guidelines, absolute risk is defined as the numerical probability of a cardiovascular event occurring within a 5-year period. This is a more accurate prediction of a person's 'individualised' risk of CVD, compared with traditional methods based on single risk factor assessments (e.g. high cholesterol, high blood pressure etc).
This release represents an important step towards improving health outcomes by establishing a more integrated approach to cardiovascular disease prevention and management in Australia. clinical decisions based on absolute CVD risk will help direct lifestyle advice and medicines to those who have the most to benefit.
New Guidelines
The Australian CVD Risk Calculator has been updated in 2023 based on NZ PREDICT-1° equation (refer to cvdcheck.org.au for more information). Pen CS is currently waiting for technical specifications from The Heart Foundation and the Department of Health to update the report algorithm based from The Framingham Risk Equation (FRE) to NZ PREDICT-1° equation. Please contact support team if have further questions.
Health professionals can access a range of related resources at http://www.cvdcheck.org.au : including the CVD online risk calculator.
The Framingham Risk Equation (FRE)
The FRE predicts the risk of a cardiovascular event over the next 5 years. The calculation can be found in the Absolute CVD Risk Resources provided at the www.cvdcheck.org.au website.
The calculation excludes patients who have:
- Age: Non ATSI <45 or >74*, ATSI <35 or >74*
- Condition: CVD
* Risk for patients who have age>74 is calculated using age=74.
The data items used in the calculation are:
- Age
- Gender
- Systolic BP (mm Hg)
- Total Cholesterol (Mg/dL)
- HDL (Mg/dL)
- Smoking Status (Smoker/Non-smoker)
- Diabetes
- ECG-LVH (always set to 0) ECG-LVH: ECG (Electrocardiogram) is a test and LVH (Left Ventricular Hypertrophy) is a condition that is detected by this test. If LVH is detected as definite this value in the FRE is set to 1, otherwise it is set to 0. Currently the outcome of this test is not recorded as a coded value in the clinical software packages and therefore cannot be extracted. Hence, this value is always set to 0.
The algorithm used is shown in this flowchart:
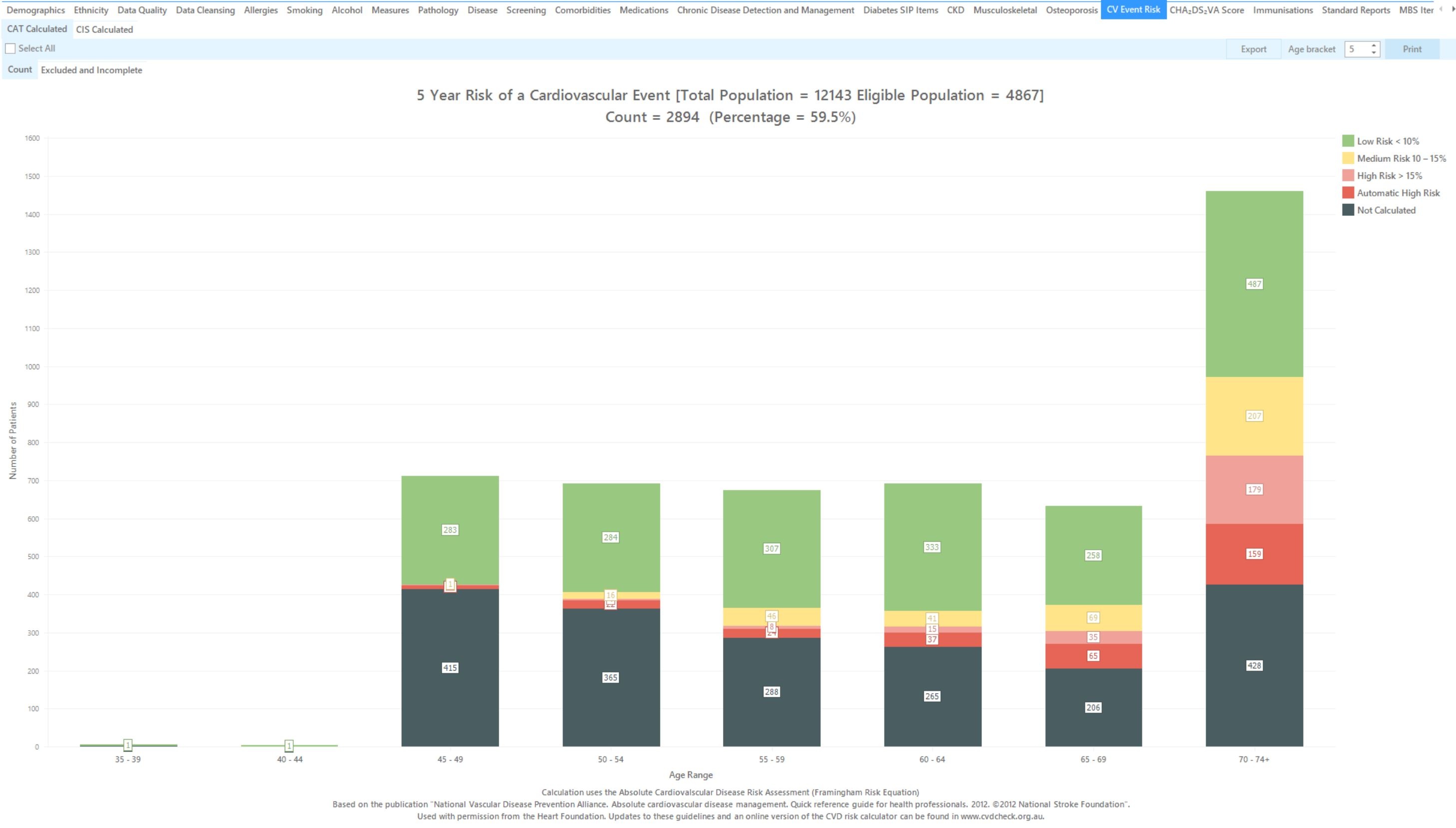
The report shows the patients who had their risk score calculated based on the Framingham equation as detailed above as well as those who had their risk automatically calculated following the flow chart shown above. Patients without a score due to incomplete data are shown as 'Not calculated', for the others the risk is displayed from low risk to high risk :
Note:
Total Population = Total population.
Eligible Population = Population who are at risk of a cardiovascular event.
Count = Population with complete data, where a risk score could be calculated.
Percentage = Count / Eligible Population.
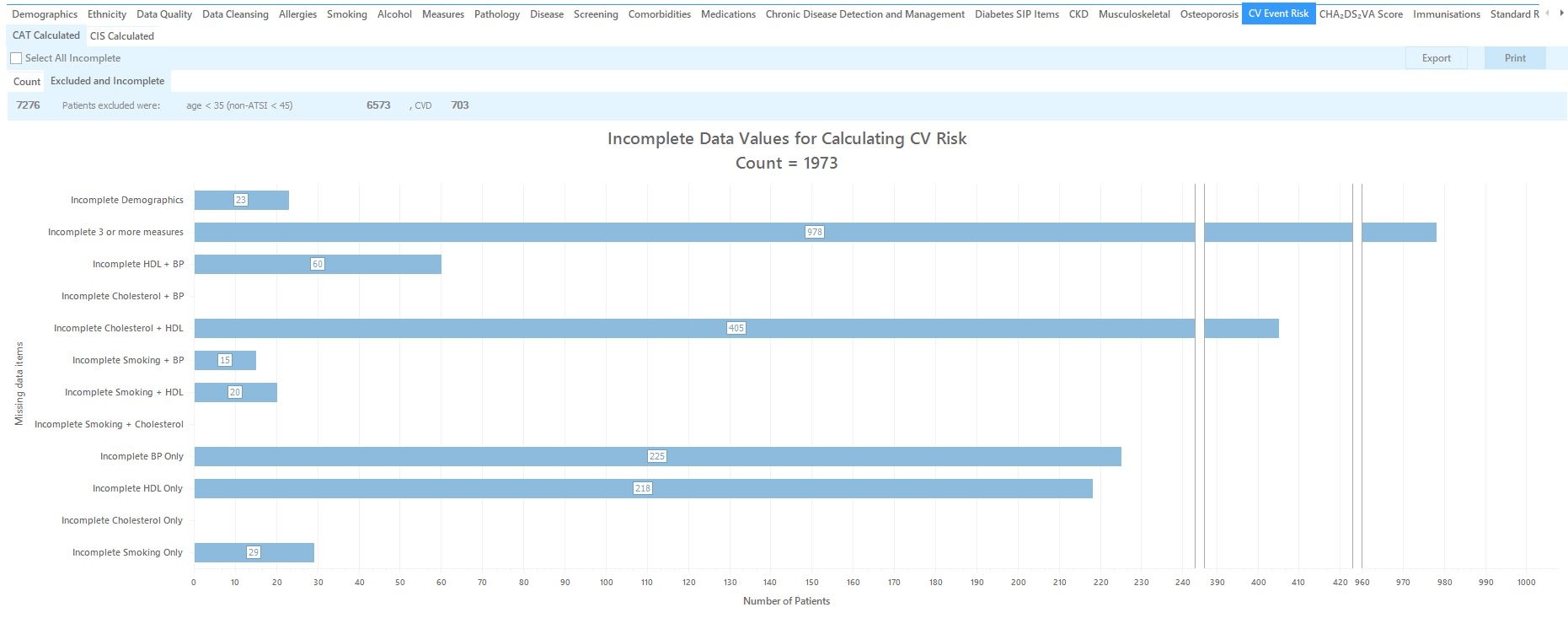
Incomplete data
This horizontal bar chart helps practice staff improve their data quality by identifying patients with missing data. The Export button can be used for this purpose as described above.
Excluded data
The number of patients that have been excluded is provided in order of exclusion category: <35 (<45 non ATSI), CVD. Once a patient is excluded for meeting an exclusion category they are not counted in subsequent categories.
Updates to these guidelines can be found at http://www.cvdcheck.org.au.